Hemorrhoids, Fissures and Tears, Oh My!
[fusion_builder_container hundred_percent=”no” equal_height_columns=”no” menu_anchor=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” id=”” background_color=”” background_image=”” background_position=”center center” background_repeat=”no-repeat” fade=”no” background_parallax=”none” parallax_speed=”0.3″ video_mp4=”” video_webm=”” video_ogv=”” video_url=”” video_aspect_ratio=”16:9″ video_loop=”yes” video_mute=”yes” overlay_color=”” video_preview_image=”” border_color=”” border_style=”solid” padding_top=”” padding_bottom=”” padding_left=”” padding_right=”” type=”legacy”][fusion_builder_row][fusion_builder_column type=”1_1″ layout=”1_1″ background_position=”left top” background_color=”” border_color=”” border_style=”solid” border_position=”all” spacing=”yes” background_image=”” background_repeat=”no-repeat” padding_top=”” padding_right=”” padding_bottom=”” padding_left=”” margin_top=”0px” margin_bottom=”0px” class=”” id=”” animation_type=”” animation_speed=”0.3″ animation_direction=”left” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” center_content=”no” last=”true” min_height=”” hover_type=”none” link=”” border_sizes_top=”” border_sizes_bottom=”” border_sizes_left=”” border_sizes_right=”” first=”true”][fusion_text columns=”” column_min_width=”” column_spacing=”” rule_style=”default” rule_size=”” rule_color=”” content_alignment_medium=”” content_alignment_small=”” content_alignment=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” sticky_display=”normal,sticky” class=”” id=”” margin_top=”” margin_right=”” margin_bottom=”” margin_left=”” font_size=”” fusion_font_family_text_font=”” fusion_font_variant_text_font=”” line_height=”” letter_spacing=”” text_color=”” animation_type=”” animation_direction=”left” animation_speed=”0.3″ animation_offset=””]
Hemorrhoids, Fissures and Tears, Oh My!
Let’s talk about something! It’s not a pleasant subject. It’s the nasty little triad of issues one might face after having a vaginal birth. I’m talking about the after-effects and trauma that can happen to your bottom. It’s rarely discussed before a birth and I believe there is a reason for that. The physical injury to the pelvic floor area from a vaginal birth can cause significant damage that leads to some rather unpleasant, uncomfortable and downright painful issues some women have to face. I’m talking about hemorrhoids, fissures, and tears that occur in the perineum during and after birth. There are some things you need to know to help you deal with these uncomfortable issues if you find you have developed these.
Hemorrhoids
Let’s start with hemorrhoids!
Hemorrhoids are a swelling and inflammation of veins in or around the anus and lower part of the rectum. They can be painful and itchy. Hemorrhoids are very common in pregnancy as the increased weight from carrying the baby causes greater pressures on the pelvic floor. Additionally, prenatal vitamins and hormones cause a slowing down of your colon and swelling of your veins, two factors contributing to constipation that can lead to hemorrhoids.
So, to avoid hemorrhoids you’ll want to avoid constipation and the bearing down that usually goes along with it.
The first step is to avoid being constipated.
Diet has a huge implication on constipation. By eating more fiber rich foods you can help keep things moving in your colon. Eating raw veggies or adding flax seeds to your food are both great ways to increase fiber intake. Be careful in adding too much fiber at first if things aren’t moving well, especially if you aren’t drinking enough water (Please consult a nutritionist for greater help with your diet).
Drinking enough water is the next step in avoiding constipation. Increasing your water intake, especially when you are breastfeeding, will bring more water to help keep things flowing through your colon. Moving your body will also do the same.
The next step it to use good toileting habits. When you sit on the toilet, you want to make sure you keep your back straight and lean forward. Avoid sitting slumped on the toilet. It can help to have your knees higher than your hips. There is the squatty potty chair you can purchase to help with this or you can use two yoga blocks, toilet paper rolls or a big fat can of tomatoes and put your feet upon them.
To relax your pelvic floor you can try making different sounds to see which sound bulges your pelvic floor downward more easily. Take a deep breath and say “Grrr!” or “Shhhh” and see which one lengthens your pelvic floor. Use that sound during your next bowel movement to help move things down and out so your pelvic floor stays relaxed!
Once a hemorrhoid is in place you need to decrease any excess pressure on this tissue in order for it to heal. With all the bearing down that happens in birth the rectal tissues need to learn to come back up in and inside again. That can only happen when you avoid bearing down during a bowel movement after your birth. It’s important to allow your stool to pass on its own without you having to force it out. Any forcefulness will only exacerbate your hemorrhoids.
Also when dealing with hemorrhoids after birth, I find you also have to address the soft tissue in your vaginal and anal openings. We’ll cover how to do this later in this article.
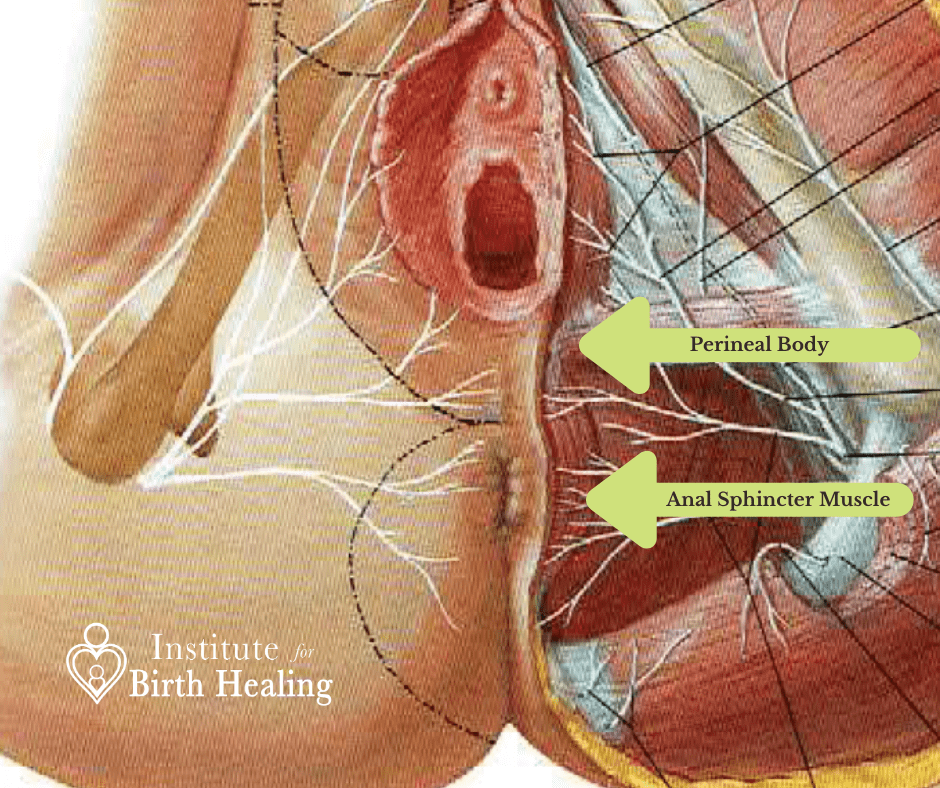
Around the anal opening is a sphincter muscle. It’s very common for this muscle to have small “knots” in it from birth, especially if you tore. These knots don’t allow the muscles to expand evenly to allow your stool to come out. When a hemorrhoid is present, most likely there is a restriction or “knot” in these tissues that can prevent hemorrhoids from healing. They can also lead to an even greater problem and that is a fissure!
Fissures
A fissure is an open tear inside the rectal tissues. Fissures have to be one of THE most painful conditions to recover from after birth. The problem with this condition is the tear has a hard time healing because it gets reopened every time you have a bowel movement. It makes having a bowel movement EXTREMELY painful! Some women, who have a fissure, report having chills, breaking out into a sweat and even their whole body shaking after having a bowel movement. The pain afterward can last for hours. When dealing with a fissure for any length of time the anticipation of a bowel movement can bring fear and greater tightness to the pelvic floor area, which creates a vicious cycle that is hard to break. It’s no fun at all!
There is one thing that has helped my clients when dealing with a fissure and that is to massage their perineum and anal sphincter prior to a bowel movement. Usually, there is increased tension in the anal sphincter that is on the opposite side of where the fissure lies. When you release this knot prior to a bowel movement it can lessen the pressures placed on the fissure and allow it to heal a little bit easier. Stay tuned to learn how to massage your anal sphincter area.
Tearing In Your Perineum
The third issue that is closely related to hemorrhoids and fissures is tearing in your perineum. Unfortunately tearing from birth is very common for women. Scar tissue forms to help heal a tear. Scar tissue is not as flexible as normal tissue and restricts tissue mobility in the area. This can inhibit a stools flow out the anal sphincter and contribute to the development and prevent the healing of hemorrhoids and fissures. Mobilizing this scar tissue can help soften the tissues and allow easier flow with less pressures, helping both issues heal.
Caring for your Perineum After Birth
So what’s a new mama to do to help her perineum after birth?
Massage this area!
What do you do? It’s simple!
Take your thumb pad and place it just inside your vaginal opening. Your first knuckle should stay on the outside. Place your index finger on the outside of your anal sphincter. Start on one side as far as you can go and pinch the two fingers together and see if it feels soft and mushy or hard and resistant to compression. You want your tissues to be soft and supple. Work your way along toward the opposite side and see where the tissues are resistant to compression. Where there is resistance you can apply pressure by gently compressing the area between your fingers while breathing into the area at the same time. Hold this pressure until you feel the tissues soften and release.
Scar tissue can create thickening and resistance to mobility. Compression and pressure can help release this but sometimes scar tissue needs more. If you find scar tissue that is not releasing to pressure there can be an emotion stuck in there. Honoring that feeling and releasing whatever emotion is there is needed before it can let go. To read more about how scar tissue and emotions are connected check out this blog post.
Pinching between the anal opening and the vagina works on the upper half of the anal sphincter. For the lower part take your index finger and apply pressure around the sphincter from 3 to 9:00 if you think of it as a clock face. Check to see if you feel any spot more resistant than the others. If you do, gently apply pressure with your finger in a downward motion and just hold it until you feel the spot release.
Massaging this area before every bowel movement can allow the tissues to expand more easily for your stool. This can help keep some of the excess pressure off your fissure area and potentially help it heal. Decreasing any resistant or thickened tissues helps to normalize the tissues so your stool flows through more easily.
There’s so much more to all of this that if you don’t find relief from doing the above, please go see a Birth Healing Specialist, women’s health physical therapist or a holistic pelvic care specialist to get some help. You can find a list of Birth Healing Specialists in the Institute For Birth Healing Directory .
[/fusion_text][/fusion_builder_column][/fusion_builder_row][/fusion_builder_container][fusion_builder_container type=”flex” hundred_percent=”no” hundred_percent_height=”no” min_height=”” hundred_percent_height_scroll=”no” align_content=”stretch” flex_align_items=”flex-start” flex_justify_content=”flex-start” flex_column_spacing=”” hundred_percent_height_center_content=”yes” equal_height_columns=”no” container_tag=”div” menu_anchor=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” status=”published” publish_date=”” class=”” id=”” link_color=”” link_hover_color=”” border_sizes=”” border_sizes_top=”” border_sizes_right=”” border_sizes_bottom=”” border_sizes_left=”” border_color=”” border_style=”solid” spacing_medium=”” margin_top_medium=”” margin_bottom_medium=”” spacing_small=”” margin_top_small=”” margin_bottom_small=”” margin_top=”” margin_bottom=”” padding_dimensions_medium=”” padding_top_medium=”” padding_right_medium=”” padding_bottom_medium=”” padding_left_medium=”” padding_dimensions_small=”” padding_top_small=”” padding_right_small=”” padding_bottom_small=”” padding_left_small=”” padding_top=”” padding_right=”” padding_bottom=”” padding_left=”” box_shadow=”no” box_shadow_vertical=”” box_shadow_horizontal=”” box_shadow_blur=”0″ box_shadow_spread=”0″ box_shadow_color=”” box_shadow_style=”” z_index=”” overflow=”” gradient_start_color=”” gradient_end_color=”” gradient_start_position=”0″ gradient_end_position=”100″ gradient_type=”linear” radial_direction=”center center” linear_angle=”180″ background_color=”” background_image=”” background_position=”center center” background_repeat=”no-repeat” fade=”no” background_parallax=”none” enable_mobile=”no” parallax_speed=”0.3″ background_blend_mode=”none” video_mp4=”” video_webm=”” video_ogv=”” video_url=”” video_aspect_ratio=”16:9″ video_loop=”yes” video_mute=”yes” video_preview_image=”” absolute=”off” absolute_devices=”small,medium,large” sticky=”off” sticky_devices=”small-visibility,medium-visibility,large-visibility” sticky_background_color=”” sticky_height=”” sticky_offset=”” sticky_transition_offset=”0″ scroll_offset=”0″ animation_type=”” animation_direction=”left” animation_speed=”0.3″ animation_offset=”” filter_hue=”0″ filter_saturation=”100″ filter_brightness=”100″ filter_contrast=”100″ filter_invert=”0″ filter_sepia=”0″ filter_opacity=”100″ filter_blur=”0″ filter_hue_hover=”0″ filter_saturation_hover=”100″ filter_brightness_hover=”100″ filter_contrast_hover=”100″ filter_invert_hover=”0″ filter_sepia_hover=”0″ filter_opacity_hover=”100″ filter_blur_hover=”0″][fusion_builder_row][fusion_builder_column type=”1_1″ layout=”1_1″ align_self=”auto” content_layout=”column” align_content=”flex-start” content_wrap=”wrap” spacing=”” center_content=”no” link=”” target=”_self” min_height=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” sticky_display=”normal,sticky” class=”” id=”” type_medium=”” type_small=”” order_medium=”0″ order_small=”0″ dimension_spacing_medium=”” dimension_spacing_small=”” dimension_spacing=”” dimension_margin_medium=”” dimension_margin_small=”” margin_top=”” margin_bottom=”” padding_medium=”” padding_small=”” padding_top=”” padding_right=”” padding_bottom=”” padding_left=”” hover_type=”none” border_sizes=”” border_color=”” border_style=”solid” border_radius=”” box_shadow=”no” dimension_box_shadow=”” box_shadow_blur=”0″ box_shadow_spread=”0″ box_shadow_color=”” box_shadow_style=”” background_type=”single” gradient_start_color=”” gradient_end_color=”” gradient_start_position=”0″ gradient_end_position=”100″ gradient_type=”linear” radial_direction=”center center” linear_angle=”180″ background_color=”” background_image=”” background_image_id=”” background_position=”left top” background_repeat=”no-repeat” background_blend_mode=”none” animation_type=”” animation_direction=”left” animation_speed=”0.3″ animation_offset=”” filter_type=”regular” filter_hue=”0″ filter_saturation=”100″ filter_brightness=”100″ filter_contrast=”100″ filter_invert=”0″ filter_sepia=”0″ filter_opacity=”100″ filter_blur=”0″ filter_hue_hover=”0″ filter_saturation_hover=”100″ filter_brightness_hover=”100″ filter_contrast_hover=”100″ filter_invert_hover=”0″ filter_sepia_hover=”0″ filter_opacity_hover=”100″ filter_blur_hover=”0″ last=”true” border_position=”all” first=”true”][fusion_tagline_box content_alignment=”left” link=”https://instituteforbirthhealing.com/six-key-assessment/” button=”DOWNLOAD NOW” linktarget=”_blank” modal=”” button_size=”” button_type=”” button_border_radius=”” buttoncolor=”default” title=”V29tZW4ncyBIZWFsdGggUHJhY3RpdGlvbmVycw==” description=”R2V0IEJldHRlciBQZWx2aWMgRmxvb3IgQ29udHJhY3Rpb25zIEluIE9ORSBTRVNTSU9OIA==” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” id=”” backgroundcolor=”” shadow=”no” shadowopacity=”0.7″ border=”1″ bordercolor=”” highlightposition=”left” margin_top=”” margin_bottom=”” animation_type=”” animation_direction=”left” animation_speed=”0.3″ animation_offset=””]
Grab the Download to Learn How Using the Six Key Assessment Tools and Techniques
[/fusion_tagline_box][/fusion_builder_column][/fusion_builder_row][/fusion_builder_container]