Diastasis Recti, What’s Really Important?
[fusion_builder_container hundred_percent=”no” equal_height_columns=”no” menu_anchor=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” id=”” background_color=”” background_image=”” background_position=”center center” background_repeat=”no-repeat” fade=”no” background_parallax=”none” parallax_speed=”0.3″ video_mp4=”” video_webm=”” video_ogv=”” video_url=”” video_aspect_ratio=”16:9″ video_loop=”yes” video_mute=”yes” overlay_color=”” video_preview_image=”” border_color=”” border_style=”solid” padding_top=”” padding_bottom=”” padding_left=”” padding_right=”” type=”legacy”][fusion_builder_row][fusion_builder_column type=”1_1″ layout=”1_1″ background_position=”left top” background_color=”” border_color=”” border_style=”solid” border_position=”all” spacing=”yes” background_image=”” background_repeat=”no-repeat” padding_top=”” padding_right=”” padding_bottom=”” padding_left=”” margin_top=”0px” margin_bottom=”0px” class=”” id=”” animation_type=”” animation_speed=”0.3″ animation_direction=”left” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” center_content=”no” last=”true” min_height=”” hover_type=”none” link=”” border_sizes_top=”” border_sizes_bottom=”” border_sizes_left=”” border_sizes_right=”” first=”true”][fusion_text columns=”” column_min_width=”” column_spacing=”” rule_style=”default” rule_size=”” rule_color=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” id=”” animation_type=”” animation_direction=”left” animation_speed=”0.3″ animation_offset=””]
I am so thrilled to see the explosion of information on Diastasis Recti (DR) on the internet. When I started working with postpartum women 11 years ago, there was a minuscule amount of material on the subject. While this swing in available information is great, I think it’s also making some people paranoid to move and not sure what to do!
So, what is really important when it comes to DR?
In this post, we’re going to take a look at my new definition of DR’s, what’s most important when assessing it, how we can try and prevent it, and most importantly how we can heal it.
FUNCTIONAL VS. DYSFUNCTIONAL DIASTASIS RECTI
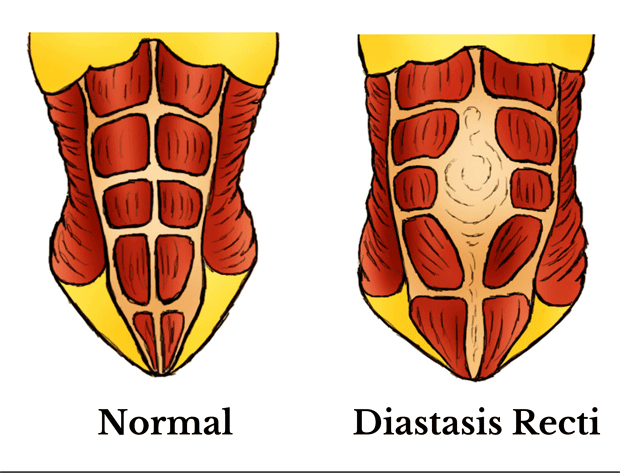
Diastasis recti are the separation of the two rectus abdominis muscle bellies that occurs as the uterus grows and puts a strain on the linea alba, the connective tissue holding the two muscles together. This is the natural design of the human body. At least 60% of women have Diastasis Recti during pregnancy.
What is so interesting about DR is the amount of separation and injury to the tissues during pregnancy varies so greatly from person to person. Some women have no separation after pregnancy, and others are left with a gaping hole in their bellies. Many factors contribute to this difference. In trying to study what is beneficial for healing, it really depends on whether someone has what I like to call a functional DR or a dysfunctional DR. The difference between the two is the amount of injury sustained to the linea alba. We need to keep in mind that normal separation between the two recti muscle bellies is between 1-2 fingers separation with shallow linea alba between. Here is what I see in my clinic and how I’ve decided to classify the wide range of separations I’ve seen.
A functional DR is less than 3 fingers separation with minimal depth to the linea alba. This type of DR usually closes on its own within the first 3 months post-birth.
A dysfunctional DR can be 3 fingers or greater and the linea alba may be displaced much deeper thus more injured and stretched out. This type of DR does not close on its own right away and takes much more effort and awareness to heal.
ASSESSMENT
While I define these two types of DR using finger width assessment, we really need to move beyond getting stuck on the width and depth of the diastasis. What is more important is the function of the tissues of the abdomen. When I’m working with my mamas, I want to make sure there is tension being generated in the linea alba when the core is being contracted. That is the telltale sign that healing can occur.
If there is no tension in the linea alba with contraction of the core, then surgery is the best option for healing. I wouldn’t go this route until you’ve stopped breastfeeding for at least a year and have worked with a qualified physical therapist or personal trainer who understands DR for up to 6 months.
When assessing the lines alba you need to do so at the belly button, a couple of inches above, and below the belly button.
PREVENTING DIASTASIS RECTI
I truly believe that DR can be prevented in most cases. If moms knew how to protect their belly during pregnancy with their movements and learn to activate their core, they could keep excess tension off the linea alba. That means avoiding any doming of the belly in the midline.
When you hug your baby into your spine with every movement and activity that requires strength, you protect your belly muscles from separation. It does require awareness and understanding of how to activate your abdominal muscles correctly.
I love teaching moms to do a long exhale to feel their lower belly tighten and drawback toward the spine as if hugging their baby back into their belly. When they get that down, then I have them practice the idea of “blow before you go!” Julie Wiebe, PT developed this concept and I love it! This means they exhale before any activity which will activate the transverse abdominus to protect the linea alba. (It’s not about blowing before you pee! :-)) It’s important to make sure this becomes an automatic response throughout pregnancy. Engagement of the belly with every movement and activity is key to helping to prevent diastasis recti during pregnancy. This engagement of your core can help you avoid any doming of the midline of your belly.
Doming means more strain on the linea able = greater separation.
Pay particular attention to how you get up and down from laying down. I wrote a 3 part blog post on preventing DR in pregnancy.
[/fusion_text][fusion_youtube id=”https://youtu.be/9zW1Fhtqnn8″ alignment=”” width=”” height=”” autoplay=”false” api_params=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” css_id=”” /][fusion_text]
Posture and how you are using your body can also contribute to creating a DR. When your lower ribcage juts forward in front of your hips this can add additional strains and forces on your abdominal tissues contributing to greater separation. Sometimes we do this to make more room for the baby as they jam up into the ribs. Learning to keep your ribcage stacked on top of your pelvis can help decrease the amount of separation of your abdominal muscles. I talk about this in the video too.
HEALING DIASTASIS RECTI
I wish there was a quick fix for healing diastasis recti. But there is not. There are however steps that can facilitate the healing process.
First and foremost is releasing the lateral abdominal muscles.
The lateral abdominal muscles, the obliques, get tight from being pregnant and can keep the recti muscles from coming back to midline. Releasing the obliques instantaneously changes the linea alba tissue and can bring more integrity to it. If every mom would do this right after birth, I know we could change the prevalence of DR! Whether you have what I call a functional DR or a dysfunctional one, releasing the obliques can really help facilitate greater healing of your abdominal wall after birth.
The next step is to work on alignment.
The abdominal wall is the connecting point between the upper body and the pelvis. In order for it to work well, we need to make sure the top part of your body, think ribcage, is stacked on top of your pelvis. This allows the abdominal muscles to work more effectively. See the above video to understand this more.
In order to heal DR, the core has to be able to engage correctly and get strong again.
Part of the core is the pelvic floor muscles. I truly wish every pregnant person could get assessed and treated by a Birth Healing Specialist. We know the steps to getting the pelvic floor muscles to activate with more strength and ease after birth. When you get things back in place, specifically the pelvic bones and organs, the muscles respond so much easier and better. You can find a practitioner in my directory on this website.
When the transverse abdominus muscle is so stretched out after birth, I like to use the pelvic floor muscles to help engage the TA. The pelvic floor muscles and TA are intimately connected as they are wired together. When you do a max contraction of one muscle, the other should contract along with it. Same for weak pelvic floor muscles, the TA can help bring it along sometimes too.
Once we have the core properly engaging, then it is all about retraining your core.
Retraining your core includes retraining it to work with each and every movement you do that requires stability of your spine. That’s almost everything you do. Opening a door, picking up the baby, even with going from sitting to standing, your lower belly should be drawing up and in with each movement.
However, how your abdominal muscles engage is critical for healing. Making sure your TA is activating from the bottom up, like in zipping up a zipper, and not your oblique muscles over-working to compensate for a weak TA. You’ll know your obliques are overactive if you notice your lower belly bulging out when you go to activate your core. Your belly button might also move downward. Ideally, the umbilicus should move backward with a slight lift up.
The next phase of healing is loading the tissues.
Now in the past, we thought that we had to be super careful with these tissues to allow them to heal. That message got out there and made moms afraid to move. We’re now aware that putting stress on the linea alba is not going to injure the tissue but instead will help to strengthen it. We still want to be aware and limit the strain that lengthens the linea alba, but doing it occasionally is not going to mess up your healing. There are a million exercises you can do to load your tissues. It’s not so important what you do but how you do it and what is happening when you do it.
Being aware of how your core engages with each and every movement is the key to healing.
This is a really quick overview of some concepts to consider when dealing with Diastasis Recti. It can be a lot more complicated than this as it all depends on how you are activating your abdominal muscles. I would just encourage anyone dealing with a DR to work with a trained professional so you can get good guidance on how you are moving and what specific exercises can help your particular situation.
[/fusion_text][/fusion_builder_column][/fusion_builder_row][/fusion_builder_container]